Analysis: The uncertain fate of patients needing life-saving dialysis treatment in Gaza
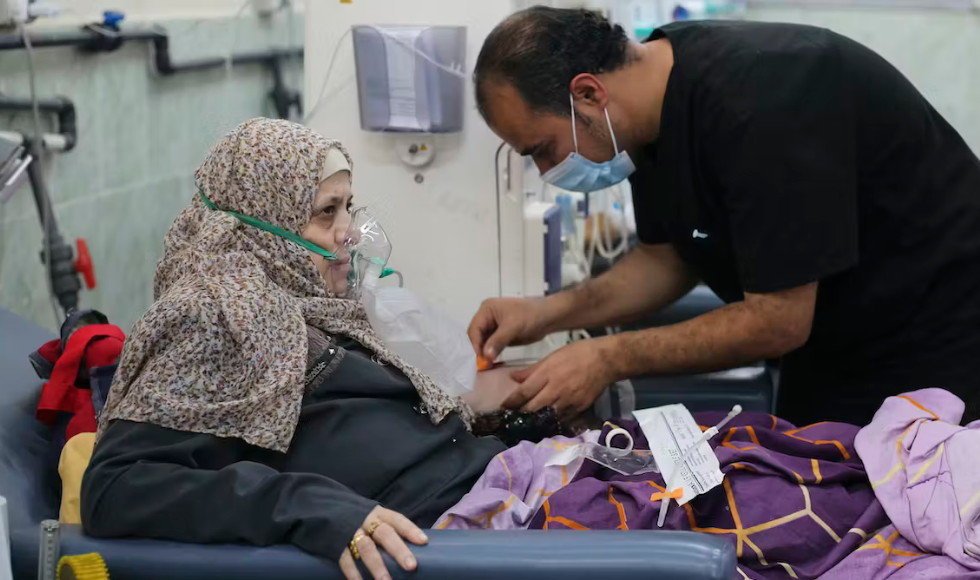
With Gaza’s health-care system crumbling amid Israel’s military assault, patients whose lives depend on dialysis are at risk with fewer and fewer facilities and resources. (AP Photo/Hatem Ali)
BY Ali Iqbal, Aliya Khan and Ben Thomson
February 6, 2024
![]() This article is republished from The Conversation under a Creative Commons license. Read the original article.
This article is republished from The Conversation under a Creative Commons license. Read the original article.
More than 100 days into the brutal assault on Gaza, over 27,000 Palestinians have been killed — of whom 60 per cent have been children and women — and 66,000 injured, according to the World Health Organization (WHO).
The destruction of Gaza’s health-care system has been catastrophic. The WHO says that, as of Jan. 5, there have been more than 600 attacks on health-care facilities, with 26 out of 36 hospitals in Gaza severely damaged and 79 ambulances targeted. Over 300 health-care workers have been killed and over 200 have been detained by Israeli forces.
In an open letter to the United Nations Security Council, Médecins Sans Frontières (MSF) president Christos Christou wrote:
“Israel has shown a blatant and total disregard for the protection of Gaza’s medical facilities. We are watching as hospitals are turned into morgues and ruins. These supposedly protected facilities are being bombed, are being shot at by tanks and guns, encircled and raided, killing patients and medical staff.”
Most of the resources within the collapsing health-care system in Gaza are directed towards treating acute trauma victims, such as the injured babies pulled from rubble, the toddlers requiring limb amputations and the civilians suffering from severe burn injuries. This leaves patients with chronic life-threatening diseases, such as cancer, heart failure and end-stage kidney disease, with severely limited access to the ongoing medical care they need to survive.
Patients unable to access care for chronic conditions

As nephrologists and internal medicine physicians, we are gravely concerned about patients in Gaza with chronic diseases who are unable to access care. There are more than 1,100 dialysis patients, including 38 children, in Gaza.
Hemodialysis is a treatment for patients with kidney failure that involves removing blood from the patient’s circulation and circulating it through a dialysis machine that clears toxins and removes excess fluid. Without adequate dialysis, fluid and toxins accumulate and patients typically die within days to weeks from respiratory failure or cardiac arrest.
Dialysis is a resource-intensive therapy that requires a dialysis facility, dialysis machines, filters, water supply and fuel, along with a team of technicians, nurses and nephrologists. Each one of these components has been severely and directly compromised since Israel’s assault on Gaza.
Israel’s complete blockade of food, fuel and water has left over 500,000 Gazans facing catastrophic hunger according to the United Nations Relief and Works Agency (UNRWA), and Gazan children face a 90 per cent reduction in access to water.
Several hospitals, including Al-Aqsa, reported being completely out of fuel, putting all patients in grave danger, particularly those on life support, babies in incubators and those requiring dialysis.
Even before the current conflict, the 16-year blockade of Gaza put the lives of kidney failure patients at risk due to chronic shortages of fuel and medical supplies. Al Jazeera reports that since Oct. 7, the number of patients at Al-Aqsa Hospital requiring dialysis has more than doubled from 143 to about 300, including 11 children, who have just 24 dialysis machines between them.
This has forced dialysis units to significantly cut treatments, with patients receiving two-hour sessions rather than the typically prescribed 3.5-hour treatments. Treatment frequency, typically prescribed three times weekly, are now only available one or two times per week.
This decrease in treatment time and frequency is grossly insufficient to sustain life. But in a health-care system under assault, patients are fortunate to receive any dialysis at all.
Patients needing life-saving treatment

Ismail Al Tawil was a 44-year-old patient in Gaza who died of kidney failure after he was unable to access dialysis. In an interview with Al-Jazeera’s AJ+ social media arm, his widow described desperately trying to get him to dialysis at Al-Shifa hospital, but being shot at by Israeli snipers who surrounded the hospital.
She then attempted to access dialysis at Al-Awda and Kamal Adwan hospitals, but both facilities had insufficient capacity to treat him.
Since Oct. 7, 1.9 million people or 85 per cent of the population of Gaza have been internally displaced, according to Human Rights Watch. This is a tremendous challenge for dialysis patients who are faced with the uncertainty of when, where or if they will access their life-saving therapy.
Anssam, age 12, was displaced from Jabaliya in northern Gaza to seek treatment in Deir El Balah in central Gaza. She had gone 15 days without dialysis and had to leave with her mother to receive life-saving medical treatment. In an interview with The National News, Anssam said:
“I hope for this war to end and for us to go back to the way we were, happy and playing, and to go back to doing dialysis three times a week… Now, without filters, I cannot have dialysis and so I will die. My life depends on dialysis.”
Loss of medical personnel
Beyond the destruction of health-care facilities and a critical shortage of supplies, the loss of medical personnel may have the most devastating and longest-lasting impact on the health-care system in Gaza.
Dr. Hammam Alloh was one of the only nephrologists in Gaza, described as a committed physician and a beacon of light by his colleagues. He was 36 years old and a father of two young children. He had hopes to expand dialysis care in Gaza and build a nephrology educational training program.
He was killed on Nov. 12 by an Israeli airstrike to his family’s home, where he was taking a short rest after a busy shift at Al Shifa Hospital. His loss resonated far beyond his family, patients and colleagues in Gaza. Dr. Alloh’s courage and dedication has become a powerful source of inspiration for physicians and health-care workers around the world.
Multiple sources have reported the number of civilians who have been killed by the bombs and bullets during the assault on Gaza. We may never know how many cancer patients will die from lack of chemotherapy; or diabetics from lack of insulin; or kidney failure patients from inadequate dialysis. The consequences of the collapsed health-care system in Gaza will be felt for years to come.
The attempts to silence, intimidate and smear health-care workers for calling out the atrocities in Gaza have been well documented. These efforts not only attempt to rob us of our freedom of speech, but of our professional and moral duty as physicians to promote global health and protect the vulnerable.
As physicians, we will not be silent as our colleagues in Gaza are being killed, as hospitals are being targeted and attacked, and as vulnerable patients are endangered. We join the UN, the WHO, MSF and the British Medical Association, along with millions around the world, who call for an immediate ceasefire and unimpeded humanitarian aid.
We stand in solidarity with the true health-care heroes of Gaza who continue to work in harrowing conditions, and we honour the legacies of those like Dr. Alloh who lost their lives while upholding the highest values of our profession.![]()
Ali Iqbal, Transplant Nephrologist, Assistant Professor of Medicine, McMaster University; Aliya Khan, Clinical professor, Faculty of Health Sciences, McMaster University, and Ben Thomson, Masters of Public Health student, Bloomberg School of Public Health, Johns Hopkins University
This article is republished from The Conversation under a Creative Commons license. Read the original article.

