A program that asks patients ‘What matters to you?’
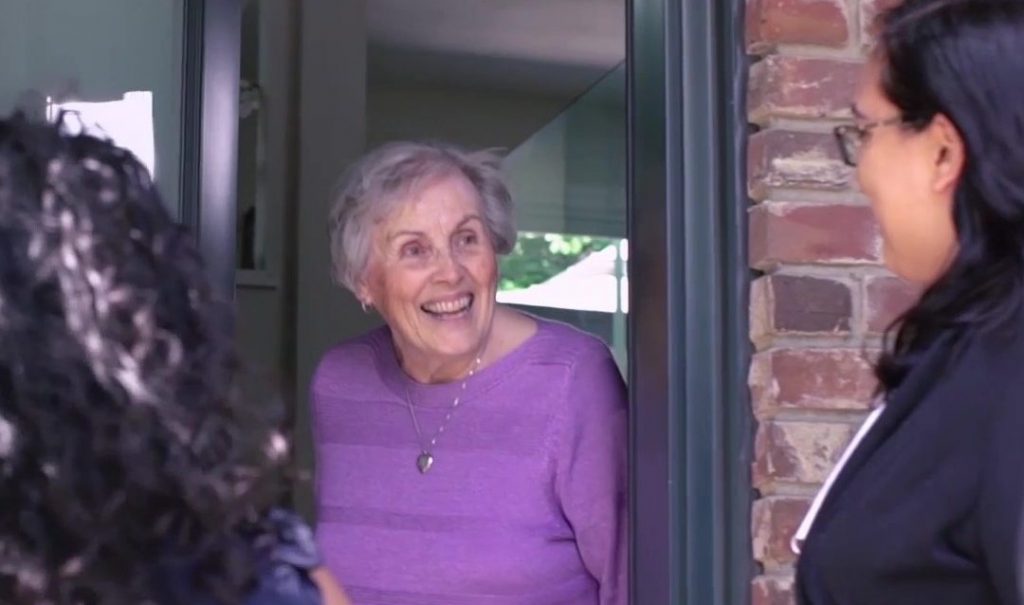
Volunteers visit older adults in their homes as part of Health TAPESTRY, an innovative program that helps people who live alone or have mobility issues receive timely and high-quality health care.
October 29, 2020
An innovative program from the department of family medicine is helping older adults, especially those who live alone or have mobility issues, receive timely and high-quality health care.
Health TAPESTRY, a community-based program, allows patients to discuss what aspects of their life and health really matter to them, leading to better health-care and health outcomes.
“We usually start our health visits by asking, ‘What’s the matter with you?’” said Doug Oliver, family physician and associate professor in the department of family medicine. “Health TAPESTRY asks, ‘What matters to you?’ and those are the gaps we’re trying to fill.”
Under the program, community volunteers visit older adults in their homes. They learn what matters most to a client, and track their health and life goals with customized software.
The volunteers then pass this information on to the client’s primary health care team, affording care providers with more insights into their patients, which leads to better health outcomes.
“When was the last time your family doctor came over to your house and had tea and really understood what was important to you?” says David Price, chair of family medicine.
“Family doctors just don’t have that kind of time, but it’s great to have that kind of information from our patients and that’s what the volunteers provide.”
The first trial of Health TAPESTRY took place in Hamilton, with promising results: older adults who participated in the program visited their primary care team more and went to the hospital less. They also spent more time walking.
In 2017, the program expanded into six Ontario communities: Sault Ste. Marie, Orangeville, Windsor, Hamilton, Niagara-on-the-Lake, and Harrow. The goal of this phase was to test whether the Health TAPESTRY approach could be adapted to other communities. This trial wrapped up in 2020 and results are forthcoming.
“We know that the health care team is critical to the health of the population, Health TAPESTRY really tries to leverage and innovate within that model,” says Dee Mangin, professor of family medicine.
“We need to stop thinking about aging as a disease and start thinking about it as a success in Canada,” Oliver says, “by allowing adults to be in charge of their own care, when their care is delivered, where it is delivered, and how it is delivered.”
Health TAPESTRY is one of several initiatives within the newly launched David Braley Primary Care Research Collaborative.


